What do you think of this article?
By Dr. David Woo - Published on August 7, 2023
Last updated on November 8, 2024
TMS, meaning Transcranial Magnetic Stimulation, is a noninvasive form of therapy used to treat a range of mental health conditions, notably depression, anxiety, attention-deficit hyperactivity disorder (ADHD), obsessive-compulsive disorder (OCD), and borderline personality disorder (BPD). The FDA has approved the marketing of TMS for the treatment of major depressive disorder (MDD), migraine headaches, and OCD, especially in cases in which pharmaceuticals have proven ineffective or intolerable (1). As TMS becomes more widely available, you may see this acronym listed as a mental health treatment option.
TMS Meaning
Cranial? Magnetic? What’s going on? Although we might not be used to hearing these words in the context of psychotherapy, they simply describe how TMS works to help regulate the causes of mental health disorders in the brain. Here’s a helpful breakdown of what TMS stands for and its meaning:
- Transcranial
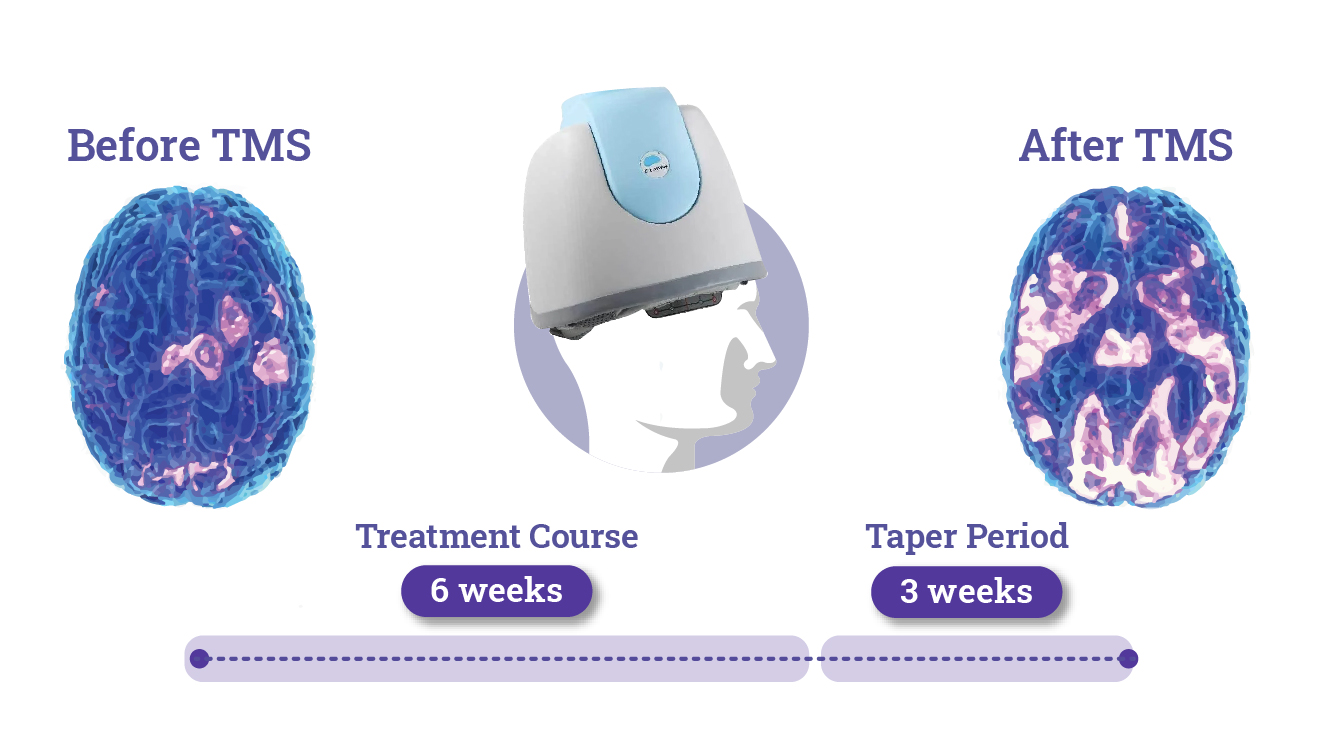
The cranium is the name given to the part of the skull that encloses and protects the brain. The prefix trans is Latin for ‘to go across’. When patients undergo TMS therapy, they wear a hat-like device called a coil. This device uses magnets to deliver tiny, barely perceptible electric charges to the brain which pass through the cranium without breaking the skin, hence transcranial.
- Magnetic
Our thoughts and emotions are generated by electrochemical activity in the brain. Electrically charged cells (neurons) ‘fire’ electrical signals that are converted into chemical messengers (neurotransmitters) that activate brain areas related to creativity , fear, self-image, logic, mood–anything that takes place inside our minds (2).
When this electrochemical activity is abnormal or imbalanced, this can lead to disrupted or unstable moods, intrusive thoughts, and other symptoms of mental disorders. The active element of TMS comes from the electromagnetic coil built into the head-mounted device. During a TMS session, the doctor will activate these magnets to send electric pulses to the brain region associated with the patient’s symptoms.
- Stimulation
The electric pulses emitted by the coil stimulate the targeted area of the brain in order to reach a healthy, balanced level of activity. For example, patients with depression often have lower-than-normal activity in the prefrontal cortex. By stimulating this region to produce more neurotransmitters, TMS helps restore brain activity to a ‘normal’, balanced level. Your doctor will determine the brain region to stimulate based on your symptoms–for example, the left side of the brain is targeted to treat depression, whereas the right side of the brain can be targeted to alleviate anxiety.
After a full course of TMS (usually six weeks), patients usually report improvements in their mood and ability to regulate their emotions as their symptoms recede. Studies have shown these positive effects to last at least a year after TMS treatment (4).
dTMS vs rTMS
You may sometimes see TMS advertised with the prefix ‘r’ or ‘d’ before the acronym. In short:
- rTMS refers to repetitive TMS, the standard form of TMS that uses repeating alternating electrical currents.
- dTMS refers to deep TMS, a more advanced form of TMS which uses specialized coils to reach wider and deeper into the brain. It is generally considered to be more effective than rTMS.
TMS Clinics in NYC
Psychiatry clinics are increasingly offering TMS therapy in addition to traditional treatments for mood disorders. If you are experiencing mental health difficulties, it is recommended to consult a doctor as soon as possible. Failure to seek medical attention may lead to a worsening of symptoms.
Madison Avenue TMS & Psychiatry offers talk therapy and TMS for treating depression, anxiety, and other mental health disorders. Contact us online or call (212) 731-2033 if you have any questions or to make an appointment.
Sources:
- FDA permits marketing of transcranial magnetic stimulation for treatment of obsessive compulsive disorder. U.S. Food & Drug Administration. Updated August 17, 2018. Link. Accessed July 17, 2023.
- How does the brain work? Dana.org. Updated August 11, 2019. Link. Accessed July 17, 2023.
- Dunner, DL, Aaronson, ST, Sackeim, HA, et al. A multisite, naturalistic, observational study of transcranial magnetic stimulation for patients with pharmacoresistant major depressive disorder: Durability of benefit over a 1-year follow-up period. The Journal of Clinical Psychiatry. 2014;75(12):1394-401. Link. Accessed July 17, 2023.
Dr. David Woo is the owner and head clinical psychiatrist at Madison Avenue TMS and Therapy in New York City. Dr. Woo has been seeing patients in private practice since 2002, always with the goals of combining evidence-based medicine with psychodynamic psychotherapy and collaborating with other mental health professionals to ensure the best possible outcomes for his patients. He has been certified to administer TMS at his practice since 2017. His greatest clinical interests include helping patients suffering from depression, anxiety, and obsessive compulsive disorder.
Follow Dr. Woo On
Dr. Woo On The Web



